How to Choose the Best Orthopedic Interlocking Nail for Surgery?
In the realm of orthopedic surgery, choosing the right device is crucial. The Orthopedic Interlocking Nail stands out as a common choice for stabilizing long bone fractures. This innovative solution provides effective support for complex injuries. However, selecting the best nail requires careful consideration of various factors.
Orthopedic Interlocking Nails come in multiple types and sizes, making the decision process complex. Factors such as fracture type, patient age, and bone quality play essential roles. Each case has unique challenges that can influence the surgical outcome. Surgeons must evaluate their experience and the specific needs of the patient. It's important to remember that not all nails fit every situation perfectly.
Understanding the nuances of different nails can enhance surgical success. Valid concerns arise from the need for proper alignment and fixation. The right Orthopedic Interlocking Nail must address patient-specific variables. This process is not merely about availability but more about reliability and efficacy in the surgical environment.
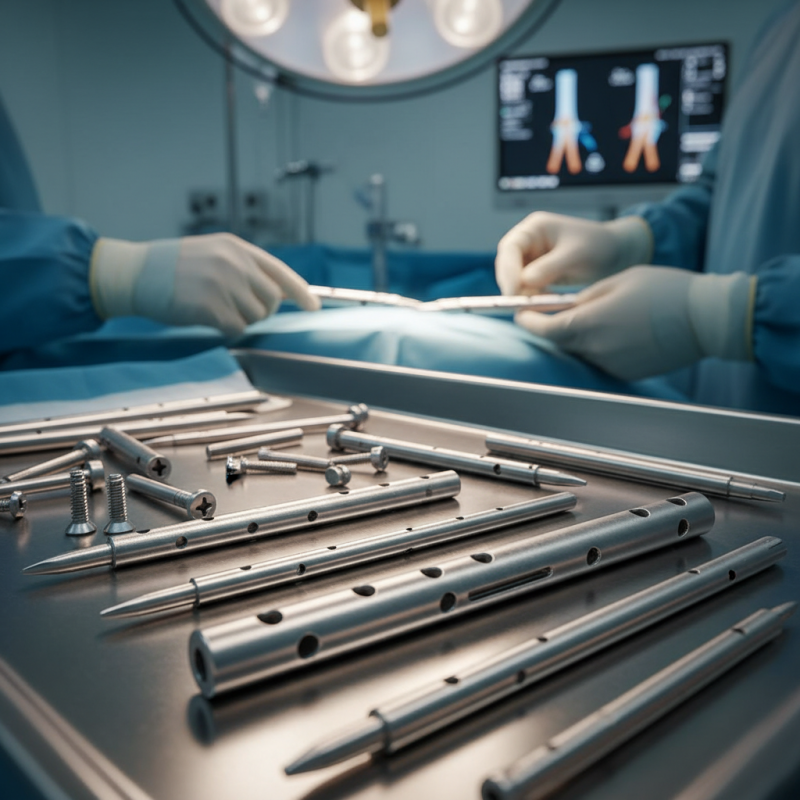
Factors to Consider When Choosing an Orthopedic Interlocking Nail
Choosing the right orthopedic interlocking nail for surgical procedures is crucial. Several factors influence this decision. The patient's age, bone condition, and fracture type are essential considerations. Surgeons must evaluate how the nail will interact with the bone and surrounding tissue. Each fracture may require a different approach.
Tip: Always assess the patient's individual needs. Customized solutions may lead to better outcomes.
The material of the interlocking nail plays a significant role too. Stainless steel and titanium are common options, but they present distinct advantages and disadvantages. Stainless steel is durable but heavier. Titanium, while lighter, can be more expensive and may not be available in all sizes. Consider the surgical environment when selecting these materials.
Tip: Consult with experienced orthopedic professionals to understand material benefits. Collaboration enhances decision-making.
Finally, ease of insertion and the design of the nail affect surgery duration. Complicated designs might save time in some cases but can complicate others. Balancing efficiency with patient safety is vital. Regularly review surgical experiences to identify patterns in nail performance.
Tip: Reflect on past surgeries to guide choices. Learning from experience is invaluable.
Types of Orthopedic Interlocking Nails and Their Uses
Orthopedic interlocking nails are essential for various types of bone fractures. Understanding the types available can guide effective surgical choices.
Intramedullary nails are widely used for long bone fractures. They provide stability and allow for early mobilization. These nails can be made from titanium or stainless steel. Each material has its pros and cons, affecting the healing process. Revisions may be needed if complications arise, such as failures in alignment.
External fixators are another option, offering stabilization from outside the body. They are useful for fractures involving infections or significant soft tissue damage. Their application may seem straightforward, yet their long-term use can come with discomfort. Surgeons must weigh the benefits against the potential for complications, such as pin site infections.
Understanding these options can empower both surgeons and patients. An in-depth discussion is vital. Fractures are unique, and individual circumstances can lead to different outcomes. Making informed decisions based on each type's characteristics is crucial for recovery.
Types of Orthopedic Interlocking Nails and Their Uses
Material Selection for Durability and Biocompatibility
Material selection is crucial for orthopedic interlocking nails. Durability and biocompatibility affect patient outcomes significantly. Studies show that titanium alloys exhibit superior strength and corrosion resistance. Reports indicate that about 90% of orthopedic implants use titanium due to its lightweight properties.
However, not all titanium is created equal. Some manufacturers may use lower-grade titanium, which can lead to implant failure. Biocompatibility is another critical factor. Materials must avoid causing adverse reactions in the human body. Research suggests that 5-10% of patients experience complications from poor material selection.
Surgeons should consider coatings that enhance biocompatibility. Hydroxyapatite coatings promote bone integration, improving long-term success rates. Yet, over-reliance on coatings can mask underlying material issues. Continuous evaluation and research are necessary to identify the best materials for orthopedic applications. Each choice carries implications for the patient's future mobility and quality of life.
Sizing and Compatibility with Patient Anatomy
When selecting an orthopedic interlocking nail, sizing and compatibility with the patient's anatomy are paramount. The correct size ensures proper alignment and stabilization. An improperly sized nail can lead to complications, such as malunion or nonunion of the fracture. Surgeons must consider bone dimensions, including length and diameter, to achieve optimal fit.
Patient anatomy varies significantly. Differences in limb length, bone density, and curvature can affect nail selection. Comprehensive imaging, like X-rays or CT scans, helps in understanding these variances. An exhaustive assessment aids in customizing the approach for each patient.
Reflection on past surgeries reveals challenges. A size too large may compromise surrounding structures. A nail that's too small can result in inadequate fixation. Continual learning from these experiences enhances decision-making. Surgeons must not only rely on standard sizing charts but also adapt to individual patient needs. The balance between technical specifications and human anatomy is crucial in orthopedic surgery.
How to Choose the Best Orthopedic Interlocking Nail for Surgery?
| Dimension | Description | Measurement (mm) | Compatibility with Patient Anatomy |
|---|---|---|---|
| Length | Total length of the nail from end to end | 300 - 450 | Match with the length of the bone |
| Diameter | Outer diameter of the nail | 8 - 12 | Adapt to the medullary canal width |
| Locking Mechanism | Type of locking that secures the nail | N/A | Ensure it fits the bone anatomy |
| Material | Composition of the nail | Titanium / Stainless Steel | Assess bone compatibility and patient allergies |
| Surface Treatment | Finish applied to the nail for better integration | Coated / Non-coated | Consider for osteointegration |
Post-Surgical Outcomes and Considerations for Nail Selection
Selecting the right orthopedic interlocking nail is crucial for successful post-surgical outcomes. The primary goal is to provide stability to the fractured bone while allowing for effective healing. Surgeons must consider the patient's age, activity level, and overall health. Each factor influences the choice of nail design and size.
Surgeons should also pay attention to potential complications. Poor nail selection might lead to issues like non-union or malunion. It’s essential to understand the specific anatomy of the injury. Some fractures may require more rigid fixation, while others might benefit from a more flexible approach. Observing previous case outcomes can provide valuable insight.
Ultimately, experience plays a significant role in nail selection. A surgeon’s familiarity with different interlocking nails can guide choices that enhance recovery. Reflecting on past surgeries can reveal areas for improvement. Each decision should stem from a blend of clinical knowledge and patient factors. An informed choice is vital for optimal healing and functional recovery.